Clinical Immunotherapy Program
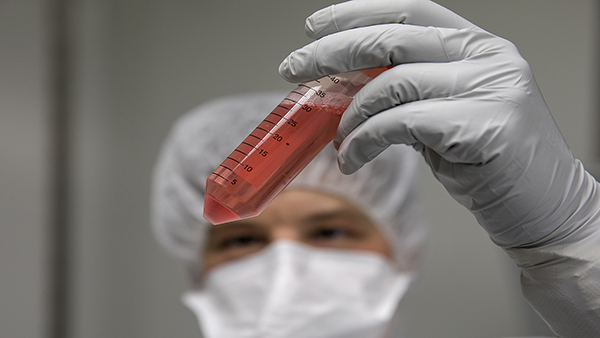

CAR-T Immunotherapy at UNC Lineberger
CAR-T immunotherapy is the re-engineering of cells from a patient’s immune system to create modified cells that are designed to recognize and direct the attack against the patient’s cancer.
Featured Publication
Journal of Clinical Oncology:
Anti-CD30 CAR-T Cell Therapy in Relapsed and Refractory Hodgkin Lymphoma
What is CAR-T immunotherapy?
The process involves extracting specific immune cells from patients, engineering the cells in the lab to hunt tumor cells displaying a specific molecular target, and then re-infusing the cells to fight a patient’s cancer.
Through the Clinical Immunotherapy Program, UNC Lineberger researchers have designed novel investigational CAR-T therapies for Hodgkin and non-Hodgkin lymphoma, multiple myeloma, neuroblastoma, leukemia, HER2 overexpressing solid tumors; and epithelial ovarian cancer that are being studied in clinical trials.

CAR-T at UNC Lineberger
UNC Lineberger is one of a select few academic centers in the United States — and the only center in North Carolina, Georgia, South Carolina, Tennessee and Virginia — with the scientific, technical and clinical capabilities to identify new tumor targets and then develop and infuse novel CAR-T immunotherapy.
These investigational therapies are manufactured at UNC Lineberger and are not commercially available; they are part of CAR-T clinical trials that are only available at UNC Lineberger in Chapel Hill, NC.
We also offer five FDA-approved, commercially available CAR-T therapies: Kymriah for acute lymphoblastic leukemia or non-Hodgkin lymphoma; Yescarta for large B-cell lymphoma and follicular lymphoma; Tecartus for mantle cell lymphoma; Breyanzi for large B-cell lymphoma; and Abecma for relapsed or refractory multiple myeloma.
Either option makes it possible for people who live in or near the Southeastern U.S. to stay closer to home to undergo clinical immunotherapy treatment for cancer.
Immuno-Oncology
During the past decade, research has shown that the immune system can be harnessed to treat multiple different types of cancer, including melanoma, lung, bladder, renal, head and neck cancers and Hodgkin’s lymphoma.
Additionally, there is increasing interest in evaluating approaches to enhance the immune response in the treatment of patients with other forms of cancer.
Researchers at the UNC Lineberger have been at the forefront of both immuno-oncology scientific research and clinical studies.
Currently, UNC Lineberger physicians have trials available using antibodies targeting immune checkpoints for patients with acute myelogenous leukemia, bladder cancer, lung cancer, and endometrial cancer. Additionally, there are trials utilizing immune therapy for the treatment of patients with sarcoma.
If you are interested in pursuing treatment on a clinical trial for these diseases, please contact the UNC Lineberger Clinical Protocol Office.
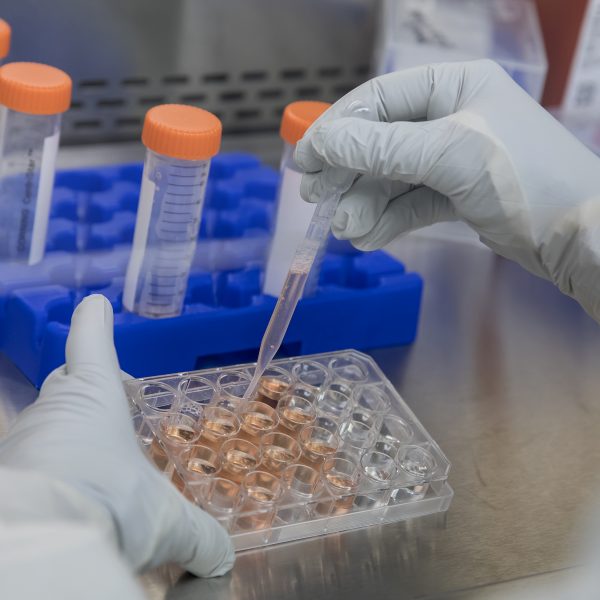
Cell Manufacturing
UNC Lineberger opened its Advanced Cellular Therapeutics Facility in 2015. The facility, which is certified to use Current Good Manufacturing Practices as set by the FDA, is located approximately five miles off campus.
Cellular therapy products are generated and expanded in this facility for patients receiving adoptive cell therapy for the treatment of cancer.
